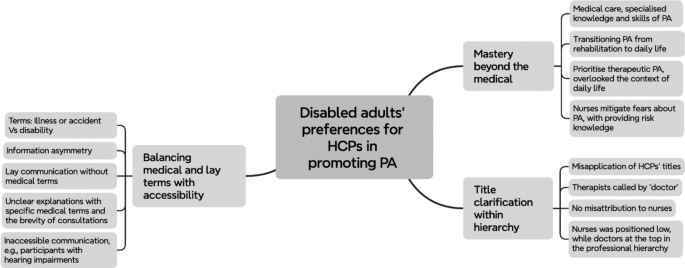
Three themes were identified: (1) mastery beyond the medical, (2) title clarification with hierarchy, and (3) balancing medical and lay terms with accessibility. These themes, generated from participants’ responses to interview questions about HCPs and their roles in promoting PA, highlight the interaction between the PAMF principles and participants’ lived experiences, while uncovering insights beyond the framework’s scope but important to understanding the roles of HCPs in PA promotion for disabled adults.
Theme 1: mastery beyond the medical
Disabled adults underscored the essential role of HCPs in providing medical care and personalised PA guidance, offering supervision and advice to support PA in the context of rehabilitation. This finding emphasises PAMF’s principles of message content and delivery. Participants who underwent rehabilitation emphasised the specialised knowledge and skills of doctors and therapists in providing good healthcare services that were focused on improving physical functions and medical conditions. As one participant said:
These doctors and therapists are all experts, which puts me at ease when performing any movement. They teach me various simple exercises to increase muscle strength and improve joint mobility. They closely monitor me as I exercise in the therapy room and promptly correct any mistakes. The movements they teach are straightforward and easy to learn. Their supervision ensures that we stay focused and do not slack off during our exercises. (XR09)
Additionally, participants emphasised that HCPs played an important role in helping disabled adults in transitioning PA from within rehabilitation to daily life. HCPs facilitated adaptive activities, defined as tailored PA designed to accommodate the specific needs of disabled individuals, such as wheelchair mobility training and balance improvement exercises, which aim to enhance disabled adults’ psychological health, confidence and independence in daily life for disabled adults. As one participant shared:
For me, this is a very important course in the Stylistics Therapy Department (Chinese:文体疗法科) at the rehabilitation centre. They taught me how to use a wheelchair in various situations, such as overcoming obstacles, going up and down slopes, and turning the wheelchair. This has allowed me to move around and start to dance again. (CC06)
However, doctors and physiotherapists tended to prioritise therapeutic PA centred on the medical condition and its clinical treatment37,38. Disabled adults felt that HCPs overlooked the importance of integrating PA into their daily lives, which is crucial for helping them transition from rehabilitation to daily activities. Some participants reported that this therapeutic PA was commonly standardised, repetitive and monotonous. This familiarity and repetition of therapeutic PA, which led to a feeling of mastery among disabled adults themselves, did not fully address disabled adults’ desire to engage in diverse and autonomy-enhancing PA. A sole focus on this therapeutic PA also diminished the credibility of HCPs from the viewpoint of disabled adults. HCPs were not deemed good sources of PA information as the professionals prescribed simply a repetitive therapeutic approach to PA. In line with one previous study16, participants were moreover reluctant to participate in this repetitive PA with HCPs due to financial issues. This gap underscores the limitations in PA message content and delivery from HCPs for disabled adults. As one participant stated:
The actions taught by the doctors (therapists) are quickly learned if you stay here a bit longer. I have been here for four years, and the new doctors (therapists) may not know as much as I do. Everyone’s treatment is more or less the same; there is no significant difference. (XR08)
I don’t want to go to the hospital often now, going to the hospital costs money, and now for me, spending money is useless. (XR10)
Additionally, nurses were noted for their crucial roles in mitigating the feeling of PA-related risk among disabled adults. Many participants expressed a fear of engaging in PA due to the potential risks and accidents, such as falls and injuries. Nurses played a crucial role in alleviating these fears by monitoring fall-related incidents and providing timely support for disabled adults within the context of rehabilitation. They worked alongside doctors and therapists, ensuring a safe and supportive environment for rehabilitation. Previous studies have highlighted the multifaceted roles of nurses in rehabilitation settings, which include assessment, coordination of care, and providing emotional support to patients39. By addressing both the physical and emotional needs of disabled adults, nurses help foster a more secure and encouraging atmosphere for engaging in PA. As participants said:
Nurses frequently inquire about our condition and caution us to exercise carefully. In contrast, doctors and therapists typically supervise our activities directly, offering immediate correction and guidance on our movements. (XR06)
These aforementioned findings highlight different roles and preferences of nurses in PA among disabled adults compared to those of doctors and therapists, which are in line with one recent study which suggested that the roles and preferences of nurses and therapists in PA were slightly different40. The study pointed out that nurses primarily focus on the patients’ rest and safety, whereas therapists are more concerned with the patients’ PA, emphasising various therapeutic activities to help patients recover and maintain physical functions40. This difference in roles and tendencies advocates a complementary dynamic in the rehabilitation process but can also present coordination challenges in PA promotion.
This theme highlights the need to expand PA delivery beyond therapeutic settings, incorporating diverse, autonomy-enhancing activities that balance safety, engagement, and practicality. While this theme aligns with PAMF’s principles of content and delivery, it also underscores the limitations of standardised therapeutic approaches and the importance of differences in the roles of HCPs in sustaining PA participation for disabled adults.
Theme 2: title clarification within a HCP hierarchy
Participants frequently expressed confusion about the titles of HCPs they interacted with, raising dilemmas in their efforts to become physically active. Participants highlighted key groups of HCPs: physiotherapists, occupational therapists, doctors and nurses. The word doctor was often incorrectly extended beyond medical doctors to include physiotherapists and occupational therapists, especially among older disabled adults living in rural areas. Participants explained using the term doctor for HCPs was a way to honour them when they could not distinguish their specific roles. As participants stated:
The best thing about being in a hospital is that doctors and nurses are around when doing exercises. I’m not sure about therapists who they are; I just call them ‘doctor’ or ‘teacher so-and-so’. (XR02)
It’d be awkward to call them (HCPs) anything else. Calling someone by their full name directly seems rude. (CC04)
As suggested, this lack of awareness about the distinct roles of physiotherapists and occupational therapists influenced their trust towards HCPs and the credibility with which they were perceived to promote PA41,42. The uncertain and often incorrect title usage influenced participants’ perceptions43, leading to misunderstandings, biases in healthcare interaction and tensions in therapeutic relationships between HCPs and patients16,43,44,45,46. This uncertainty and misapplication resulted in ineffective PA promotion by HCPs for disabled adults. Clear identification of what each HCP is about and does is crucial to minimise this misapplication and enable disabled people to make informed healthcare decisions43. These findings emphasise the importance of clarity in HCPs’ titles for disabled adults’ PA participation, which could be useful in building positive therapeutic relationships between HCPs and disabled adults.
However, the uncertainty and misattribution of titles did not extend to nurses. Participants explained that nurses were mostly women and wore distinct uniforms that helped distinguish their identification from other HCPs. As participants stated:
If a nurse is an expert, I will listen to their advice on PA. But if I were to compare, I would give precedence to the doctor’s advice. (XR06)
Nurses are easy to know. They had hats and wore different clothes from others. (CC04)
This perceived hierarchy among HCPs, which places nurses in a subordinate role compared to doctors and therapists, aligns with previous studies in the context of rehabilitation47,48. This subordinate perception of nurses could negatively impact the efficacy of rehabilitation and PA promotion efforts by nurses among disabled adults.
This theme aligns with the PAMF’s focus on messenger identity, highlighting how the roles and credibility of HCPs shape the effectiveness of PA promotion among disabled adults. Misattributions and unclear role identification undermine the perceived credibility of HCPs, hindering their capacity to deliver impactful PA messages. While not directly aligned with the PAMF’s predefined components, these findings offer critical insights into how role ambiguity and hierarchical perceptions influence trust in HCPs. Addressing these challenges requires efforts to enhance awareness of HCP identities and contributions to improve PA promotion and build positive therapeutic relationships among disabled adults. Furthermore, challenging medical hierarchies remains an important task in PA promotion.
Theme 3: balancing medical and Lay terms with accessibility
Disabled adults held different preferences for disability-related terms when communicating with HCPs that impacted on their PA participation. Participants had a preference for terms, such as illness or accident over disability when discussing PA with HCPs within rehabilitation contexts. This preference reflected a reluctance to accept their disability and an optimism towards recovery, especially during the early stage of rehabilitation or the transitional period from medical care to societal settings. The use of these medical terms underscored the influences of medical models of disability on PA promotion within healthcare contexts. As one participant stated:
I am a patient. Since I got the illness, I’ve been consistently exercising. Keeping doing exercise, I may recover completely one day. There may be a miracle. (XR09)
In contrast, some participants, who had not experienced rehabilitation, resisted being labelled a patient from HCPs, suggesting a preference for the social model of disability over the medical model of disability. Scullion critiqued these medicalised labels by HCPs, such as patients, arguing that they negatively impacted the self-identity of disabled individuals during the transitional phases by reinforcing a weakened self-perception in line with the medical model of disability49. In the words of one participant:
You go to the hospital when you are sick or seriously ill. I am disabled, not ill. I am not a patient to do exercise. So I do not frequently prefer HCPs in PA participation. (CC23)
These different preferences for disability-related terms indicate varying attitudes towards disability among disabled adults, reflecting a divergence in self-perception and identity during different disability phases. These varying attitudes towards disability among disabled adults underscore the necessity for HCPs to use appropriate disability-related terms in promoting PA for disabled adults, tailored to the different phases of disability they experienced. As participants stated:
I come back here every year for rehabilitation after my illness. It’s been three or four years now. I am a patient not like normal persons. I take the initiative to exercise more here. Those healthcare workers call me uncle; it motivates me to stay here. (XR09)
I became disabled because of an accident when I was very young. It’s been many years now, and I only see a doctor when I’m sick. I’m not a patient, and I don’t want to go to the hospital. If I were to consult about exercise, I wouldn’t want to be treated as a patient or be told I have an illness. Being referred to in a non-medical way encourages me to stay active. (CC04)
Participants also emphasised the need for lay language in communicating about PA with HCPs in rehabilitation contexts. Effective lay communication was suggested to foster positive relationships between HCPs and disabled adults, creating an inclusive environment in rehabilitation settings. This inclusive environment was highly valued by disabled adults as it enhanced their sense of belonging and trust with HCPs in rehabilitation settings, influencing disabled adults’ decision to participate in PA and extend their stay in rehabilitation settings. As participants explained:
Doctors and therapists work very seriously and have a good attitude. I can ask them anything I don’t understand when I am doing exercise in the rehabilitation department. They have the patience to answer my questions and listen to me during my exercises. I do exercise every day except for Sunday. There is no discrimination here. Everyone around is similar. In the beginning, I couldn’t accept the reality of my disability. I met so many people in the same situation in the hospital. I realised that I’m not the only one like this in the world. At home, there is no such environment without discrimination. Sometimes we train together and have chats. We feel like family together. Actually, the hospital environment had a significant impact on me. (CC06)
The doctors are busy and don’t have enough time to answer questions. Sometimes we don’t understand the professional terms the doctors use, sometimes they are in English. We haven’t been educated, we don’t understand. In the therapy room, after getting to know the therapists, sometimes we ask questions while they are treating other patients, but we definitely can’t do that every day. (XR09)
These quotes highlight the importance of effective lay language in building trust and positive relationships between HCPs and disabled adults for promoting PA. One previous study found that therapeutic relationships were often tense due to inadequate communication and a lack of effective conflict mediation in public hospitals in China16. The absence of effective lay language, coupled with the complexity of medical terms and brief consultation with unclear explanations from HCPs, can exacerbate information asymmetry and misunderstandings among disabled adults, reducing the effectiveness of PA promotion they suggested. Therefore, it is important for HCPs to use lay languages and create inclusive environments to support disabled adults in PA participation in China.
Regarding the inclusive environment for promoting PA, accessibility is an important factor for effective communication between HCPs and disabled adults. Participants with hearing impairments particularly emphasised the difficulties they faced in accessing communication with HCPs in PA participation, such as the need for sign language assistance. This inaccessibility in communicating with HCPs is compounded by logistical challenges, such as online registration and the high cost of medical treatment and services. As participants stated:
Going to the hospital is quite inconvenient; you have to register, and now many registrations have to be done online or on a machine by yourself. There might be nurses to help with registration, but they are very busy; sometimes one person has to help many people. For us with hearing impairments, going to the hospital is actually more troublesome, the doctors also can’t understand our sign language, and we can’t speak out. (CC28)
Registration costs money. If possible, we still hope to have some free consultations with doctors in the community to help us out. (XR09)
This theme reflected PAMF’s focus on message framing and inclusive communication, which also revealed the deeper impact of terminology on identity and trust. Factors, such as information asymmetry, economic issues, and the dominance of the medical model of disability, influence the effectiveness of communication between HCPs and disabled adults. These findings revealed limitations in PAMF’s practical application, addressing systematic barriers such as financial issues. Communication barriers, such as the use of complex medical terms and brief consultations, coupled with logistical challenges like online registration and high treatment costs, further exacerbate these issues. To address these challenges, more accessible, community-based healthcare consultations should be developed to reduce financial barriers and be tailored to the specific needs of disabled adults. These solutions could include subsidised healthcare services, and financial assistance programs to offer low-cost or free consultations. By addressing these barriers and promoting effective lay communication, HCPs can better support PA participation among disabled adults, fostering a more inclusive and accessible environment for disabled adults to promote PA.
Strengths and limitations
This study is the first qualitative investigation into disabled adults’ preferences for how HCPs promote PA within the context of China. A key strength of this research is its novelty. By focusing on disabled adults in China, this study offers original evidence to support PA promotion in healthcare settings. The insights gathered from participants shed light on their perceptions and experiences with HCPs, highlighting the potential role of these professionals in promoting PA. Additionally, these insights suggest potential ways to strengthen therapeutic relationships between healthcare professionals and patients in China.
The authors acknowledge several limitations of the study. The sample, consisting of a convenience group of disabled adults, was predominantly from Eastern mainland China. The recruitment period and online interview methods restricted the sample size, particularly among adults with mental illnesses. This limitation may have resulted in a selection bias, with more motivated individuals sharing their experiences. Future research should aim for a more diverse sample, including a broader range of disabled adults and geographic areas, particularly those with mental illnesses, to provide a more comprehensive insight.
link